ICG Dosing and Timing for Breast Cancer Surgery
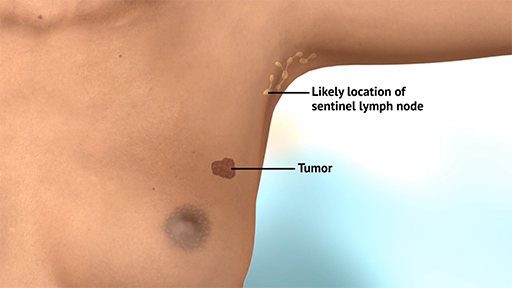
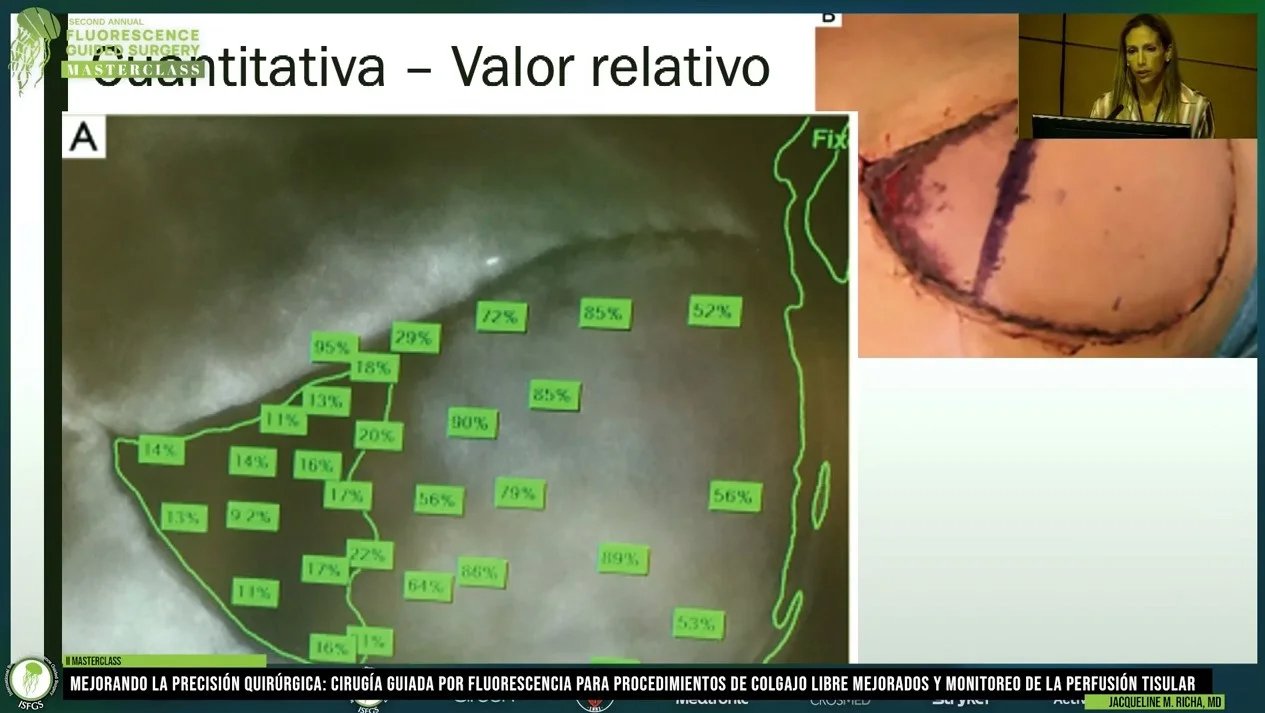
Indocyanine green (ICG) fluorescence imaging is increasingly used in breast cancer surgery to visualize lymphatic drainage, identify sentinel lymph nodes, and assess tissue perfusion during reconstruction. Proper dosing and timing of ICG administration are essential to achieve optimal near-infrared fluorescence imaging during the procedure.
This dosing and timing chart provides practical guidance for ICG use in breast cancer surgery, including recommended injection techniques, dosage ranges, and expected fluorescence detection times for sentinel lymph node mapping and breast reconstruction perfusion assessment.
Purpose: | Visualize lymphatic drainage & sentinel lymph node |
Injection Type: | Other |
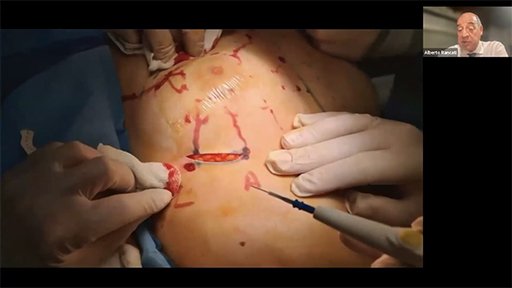
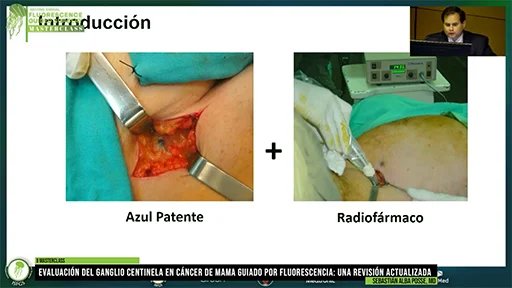
Description: | Dye administration should be subcutaneous into periareolar region of each quadrant. |
Dilution (25 mg in 10 mL of sterile water - 2.5mg/mL): | Yes |
Requires Flush with Sterile Water: | No |
Proposed Dosage: | 1 mL |
Injection Time: | At start of procedure. |
First Indocyanine Green Detection: | Five to 10 minutes after administration |
Indocyanine Green Duration: | Stable during surgery. Slowly diffuses through lymphatics |
Camera Requirements (handheld device, laparoscope or both): | Handheld |
Tips & Tricks: | Total 4 mL (1 mL per periareolar quadrant). Gentle, circular motion massaging can be performed to distribute dye. |
SPECIAL CONSIDERATIONS
- ALWAYS dilute with sterile water
- ALWAYS flush with normal saline
- Max dose is 2 mg/kg (e.g.: 120 mg or 4.8 reconstituted flasks of 25 mg/mL of ICG)
- *For 0.1 and 0.2 mL doses, utilize an insulin syringe to draw/administer volumen.
DISCLAIMERS
- Doses are device-dependent
- The above dosage and timing information have been collated from worldwide surgeons expert in these procedures and is based on their recommendations and is not evidence-based.
- All dosages have been adjusted to the U.S. recommended dilution of 25mg of ICG in 10mL of sterile water
- Approval for listed indications may vary according to country.
- Dip F, LoMenzo E, Sarotto L, et al. Randomized Trial of Near-infrared Incisionless Fluorescent Cholangiography. Ann Surg. 2019;270(6):992-999. doi:10.1097/SLA.0000000000003178
- Symeonidis S, Mantzoros I, Anestiadou E, et al. Biliary Anatomy Visualization and Surgeon Satisfaction Using Standard Cholangiography versus Indocyanine Green Fluorescent Cholangiography during Elective Laparoscopic Cholecystectomy: A Randomized Controlled Trial. J Clin Med. 2024;13(3):864. Published 2024 Feb 1. doi:10.3390/jcm13030864
- Ishizawa T, McCulloch P, Stassen L, et al. Assessing the development status of intraoperative fluorescence imaging for anatomy visualisation, using the IDEAL framework. BMJ Surg Interv Health Technol. 2022;4(1):e000156. Published 2022 Nov 4. doi:10.1136/bmjsit-2022-000156
- Shen Y, Yang T, Yang J, Meng W, Wang Z. Intraoperative indocyanine green fluorescence angiography to prevent anastomotic leak after low anterior resection for rectal cancer: a meta-analysis. ANZ J Surg. 2020;90(11):2193-2200. doi:10.1111/ans.15809
- Lucarini A, Guida AM, Orville M, Panis Y. Indocyanine green fluorescence angiography could reduce the risk of anastomotic leakage in rectal cancer surgery: a systematic review and meta-analysis of randomized controlled trials. Colorectal Dis. 2024;26(3):408-416. doi:10.1111/codi.16868
- Rinne JKA, Huhta H, Pinta T, et al. Indocyanine Green Fluorescence Imaging in Prevention of Colorectal Anastomotic Leakage: A Randomized Clinical Trial. JAMA Surg. Published online March 5, 2025. doi:10.1001/jamasurg.2025.0006
- Felli E, Ishizawa T, Cherkaoui Z, et al. Laparoscopic anatomical liver resection for malignancies using positive or negative staining technique with intraoperative indocyanine green-fluorescence imaging. HPB (Oxford). 2021;23(11):1647-1655. doi:10.1016/j.hpb.2021.05.006
- Alomari MAM, Wakabayashi T, Colella M, et al. Comparing the accuracy of positive and negative indocyanine green staining in guiding laparoscopic anatomical liver resection: protocol for a randomised controlled trial [published correction appears in BMJ Open. 2023 Dec 12;13(12):e072926corr1. doi: 10.1136/bmjopen-2023-072926corr1.]. BMJ Open. 2023;13(9):e072926. Published 2023 Sep 20. doi:10.1136/bmjopen-2023-072926
- Wakabayashi T, Cacciaguerra AB, Abe Y, et al. Indocyanine Green Fluorescence Navigation in Liver Surgery: A Systematic Review on Dose and Timing of Administration. Ann Surg. 2022;275(6):1025-1034. doi:10.1097/SLA.0000000000005406
- Zhou K, Zhou S, Du L, et al. Safety and effectiveness of indocyanine green fluorescence imaging-guided laparoscopic hepatectomy for hepatic tumor: a systematic review and meta-analysis. Front Oncol. 2024;13:1309593. Published 2024 Jan 3. doi:10.3389/fonc.2023.1309593
- Liu F, Wang H, Ma W, et al. Short- and Long-Term Outcomes of Indocyanine Green Fluorescence Navigation- Versus Conventional-Laparoscopic Hepatectomy for Hepatocellular Carcinoma: A Propensity Score-Matched, Retrospective, Cohort Study. Ann Surg Oncol. 2023;30(4):1991-2002. doi:10.1245/s10434-022-13027-5
- Liberale G, Bourgeois P, Larsimont D, Moreau M, Donckier V, Ishizawa T. Indocyanine green fluorescence-guided surgery after IV injection in metastatic colorectal cancer: A systematic review. Eur J Surg Oncol. 2017;43(9):1656-1667. doi:10.1016/j.ejso.2017.04.015
- Sakuma J, Hoshino A, Fujiwara H, et al. Blood flow assessment of gastric tube with indocyanine green fluorescence angiography and postoperative endoscopy during esophagectomy: indocyanine green enhancement time indicated congestion. BMC Gastroenterol. 2024;24(1):316. Published 2024 Sep 17. doi:10.1186/s12876-024-03398-2
- Sozzi A, Bona D, Yeow M, et al. Does Indocyanine Green Utilization during Esophagectomy Prevent Anastomotic Leaks? Systematic Review and Meta-Analysis. J Clin Med. 2024;13(16):4899. Published 2024 Aug 20. doi:10.3390/jcm13164899
- Pather K, Deladisma AM, Guerrier C, Kriley IR, Awad ZT. Indocyanine green perfusion assessment of the gastric conduit in minimally invasive Ivor Lewis esophagectomy. Surg Endosc. 2022;36(2):896-903. doi:10.1007/s00464-021-08346-9
- Song HC, Wu MH, Liu JX, et al. Retrograde transurethral injection of indocyanine green better assists complete transperitoneal nephroureterectomy in a single-position. Transl Androl Urol. 2024;13(9):1868-1877. doi:10.21037/tau-24-247
- Centini G, Colombi I, Cannoni A, et al. Systematic use of intraureteral indocyanine green: a game changer in endometriosis surgery. A proof-of-concept study. Minim Invasive Ther Allied Technol. 2024;33(5):287-294. doi:10.1080/13645706.2024.2386658
- White LA, Joseph JP, Yang DY, et al. Intraureteral indocyanine green augments ureteral identification and avoidance during complex robotic-assisted colorectal surgery. Colorectal Dis. 2021;23(3):718-723. doi:10.1111/codi.15407
- White LA, Joseph JP, Yang DY, et al. Intraureteral indocyanine green augments ureteral identification and avoidance during complex robotic-assisted colorectal surgery. Colorectal Dis. 2021;23(3):718-723. doi:10.1111/codi.15407
- Spartalis E, Ntokos G, Georgiou K, et al. Intraoperative Indocyanine Green (ICG) Angiography for the Identification of the Parathyroid Glands: Current Evidence and Future Perspectives. In Vivo. 2020;34(1):23-32. doi:10.21873/invivo.11741
- Zhang D, Sun H, Frattini F, et al. Use of Indocyanine Green Fluorescence During Total Thyroidectomy to Identify Parathyroid Glands and Prevent Hypoparathyroidism. Surg Technol Int. 2022;43:77-82. doi:10.52198/23.STI.43.GS1741
- Brezgyte G, Mills M, van Zanten M, Gordon K, Mortimer PS, Ostergaard P. A systematic review of indocyanine green lymphography imaging for the diagnosis of primary lymphoedema. Br J Radiol. 2025;98(1168):517-526. doi:10.1093/bjr/tqaf006
- Peristeri DV, Baltatzis M. Real-Time Fluorescence Imaging for Thoracic Duct Identification during Oesophagectomy: A Systematic Review of the Literature. J Chest Surg. 2025;58(1):5-14. doi:10.5090/jcs.24.091
- Jupitz SA, Lin C, Kawahara T, McKinney G, Uselmann AJ, Neuman HB. Higher Rates of Visualization for Axillary Reverse Mapping Using Indocyanine Green Fluorescence Compared With Blue Dye. J Surg Res. 2025;306:290-298. doi:10.1016/j.jss.2024.11.043
- Koh KML, Ng ZY, Chin FHX, Wong WL, Wang J, Lim YK. Comparing Surgical and Oncological Outcomes between Indocyanine Green (ICG) Sentinel Lymph Node Mapping with Routine Lymphadenectomy in the Surgical Staging of Early-Stage Endometrioid Endometrial Cancer. Obstet Gynecol Int. 2023;2023:9949604. Published 2023 Oct 17. doi:10.1155/2023/9949604
- Papadia A, Imboden S, Siegenthaler F, et al. Laparoscopic Indocyanine Green Sentinel Lymph Node Mapping in Endometrial Cancer. Ann Surg Oncol. 2016;23(7):2206-2211. doi:10.1245/s10434-016-5090-x
- Holloway RW, Gupta S, Stavitzski NM, et al. Sentinel lymph node mapping with staging lymphadenectomy for patients with endometrial cancer increases the detection of metastasis. Gynecol Oncol. 2016;141(2):206-210. doi:10.1016/j.ygyno.2016.02.018
- Koual M, Benoit L, Nguyen-Xuan HT, Bentivegna E, Azaïs H, Bats AS. Diagnostic value of indocyanine green fluorescence guided sentinel lymph node biopsy in vulvar cancer: A systematic review. Gynecol Oncol. 2021;161(2):436-441. doi:10.1016/j.ygyno.2021.01.031
- Verbeek FP, Tummers QR, Rietbergen DD, et al. Sentinel Lymph Node Biopsy in Vulvar Cancer Using Combined Radioactive and Fluorescence Guidance. Int J Gynecol Cancer. 2015;25(6):1086-1093. doi:10.1097/IGC.0000000000000419
- Kodama K, Tateishi C, Oda T, et al. Development of novel tracers for sentinel node identification in cervical cancer. Cancer Sci. 2023;114(11):4216-4224. doi:10.1111/cas.15927
- Pop FC, Veys I, Vankerckhove S, et al. Absence of residual fluorescence in the surgical bed at near-infrared fluorescence imaging predicts negative margins at final pathology in patients treated with breast-conserving surgery for breast cancer. Eur J Surg Oncol. 2021;47(2):269-275. doi:10.1016/j.ejso.2020.09.036
- Wang P, Shuai J, Leng Z, Ji Y. Meta-analysis of the application value of indocyanine green fluorescence imaging in guiding sentinel lymph node biopsy for breast cancer. Photodiagnosis Photodyn Ther. 2023;43:103742. doi:10.1016/j.pdpdt.2023.103742
- López Gordo S, Borisova I, Ruiz-Edo N, et al. Indocyanine green for axillary sentinel lymph node biopsy in patients with breast cancer (INSEAN study). Cir Esp (Engl Ed). 2025;103(3):173-178. doi:10.1016/j.cireng.2024.11.017
- Lee JK, Jeon BJ, Woo KJ. Ingress Time as a Metric for Indocyanine Green Angiographic Evaluation of Skin Flap Perfusion in Immediate Implant-Based Reconstruction. Plast Reconstr Surg. Published online February 11, 2025. doi:10.1097/PRS.0000000000012034
- Nguyen CL, Dayaratna N, Easwaralingam N, et al. Developing an Indocyanine Green Angiography Protocol for Predicting Flap Necrosis During Breast Reconstruction. Surg Innov. 2025;32(2):77-84. doi:10.1177/15533506241313172
- Wölffer M, Liechti R, Constantinescu M, Lese I, Zubler C. Sentinel Lymph Node Detection in Cutaneous Melanoma Using Indocyanine Green-Based Near-Infrared Fluorescence Imaging: A Systematic Review and Meta-Analysis. Cancers (Basel). 2024;16(14):2523. Published 2024 Jul 12. doi:10.3390/cancers16142523
- Lafreniere AS, Shine JJ, Nicholas CR, Temple-Oberle CF. The use of indocyanine green and near-infrared fluorescence imaging to assist sentinel lymph node biopsy in cutaneous melanoma: A systematic review. Eur J Surg Oncol. 2021;47(5):935-941. doi:10.1016/j.ejso.2020.10.027
- Knackstedt RW, Couto RA, Gastman B. Indocyanine green fluorescence imaging with lymphoscintigraphy for sentinel node biopsy in head and neck melanoma. J Surg Res. 2018;228:77-83. doi:10.1016/j.jss.2018.02.064